 Enthesopathy (inflammation of ligaments or tendons).Enthesitis (inflammation of entheses, where tendons attach to bone).Bursitis (inflammation of soft tissues).Bone marrow edema (inflammation of bone marrow).Active sacroiliitis not yet visible on X-rays.The same bone changes seen on X-rays, as well as early cartilage abnormalities and erosions.MRI is a sensitive test that uses magnetic energy to detect active inflammatory changes in early spondylitis. MRI is also safer than X-ray because it does not emit radiation. Early diagnosis allows for early intervention, which may help prevent long-term damage caused by spondylitis. Using an MRI, a doctor can diagnose nonradiographic spondylitis before it becomes radiographic. MRI can help the diagnostic accuracy of early spondylitis because it can detect inflammation before it causes damage that’s visible on an X-ray. MRI is the imaging test ordered when changes are not detected by X-ray in a person suspected to have spondylitis. Still, X-rays play an important role in tracking spondylitis progression because they are easily accessible, yield quick results, and remain the standard for capturing bone changes. It can take two years or more between X-rays for radiologists to detect disease progression. They are also more accessible than magnetic resonance imaging (MRI) because they are quicker, less expensive, and have shorter wait times. X-rays emit less radiation than computerized tomography (CT) scans, another imaging test option. Subchondral sclerosis (thickening of bone in joints).Ossification (new bone formation between the vertebrae).Syndesmophytes, osteophytes, spondylophytes, and enthesophytes (types of bone spurs or growths).Joint damage and erosion from inflammation (evidence of sacroiliitis). 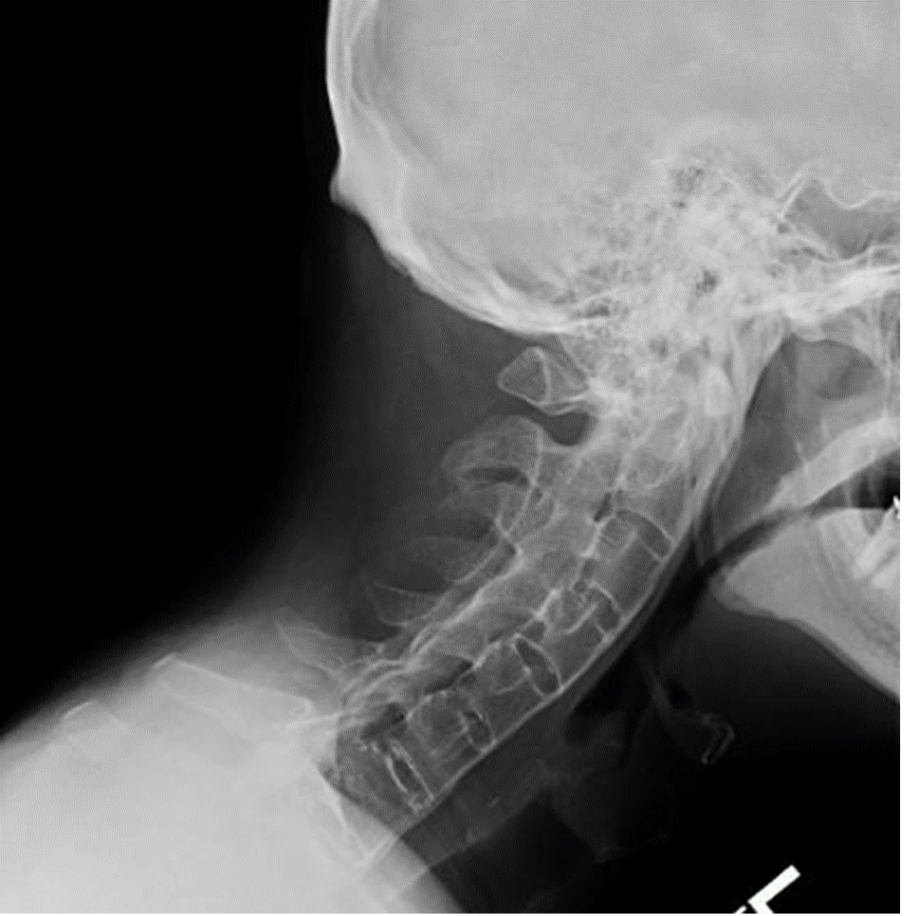
Some of the bone changes typical of spondylitis that may be detected by X-ray include: Spondylitis inflammation usually attacks the sacroiliac joints first, causing sacroiliitis. Radiographic images can be used to help diagnose radiographic spondylitis, or ankylosing spondylitis, by detecting bone changes. Why imaging is vital for early detection of axial spondyloarthritis It can sometimes take five years or more from disease onset for changes caused by spondylitis to be detected by an X-ray. X-rays pick up bone changes caused by inflammation rather than early disease activity present in soft tissues. A notable disadvantage to X-rays is that they do not detect early disease activity, however.  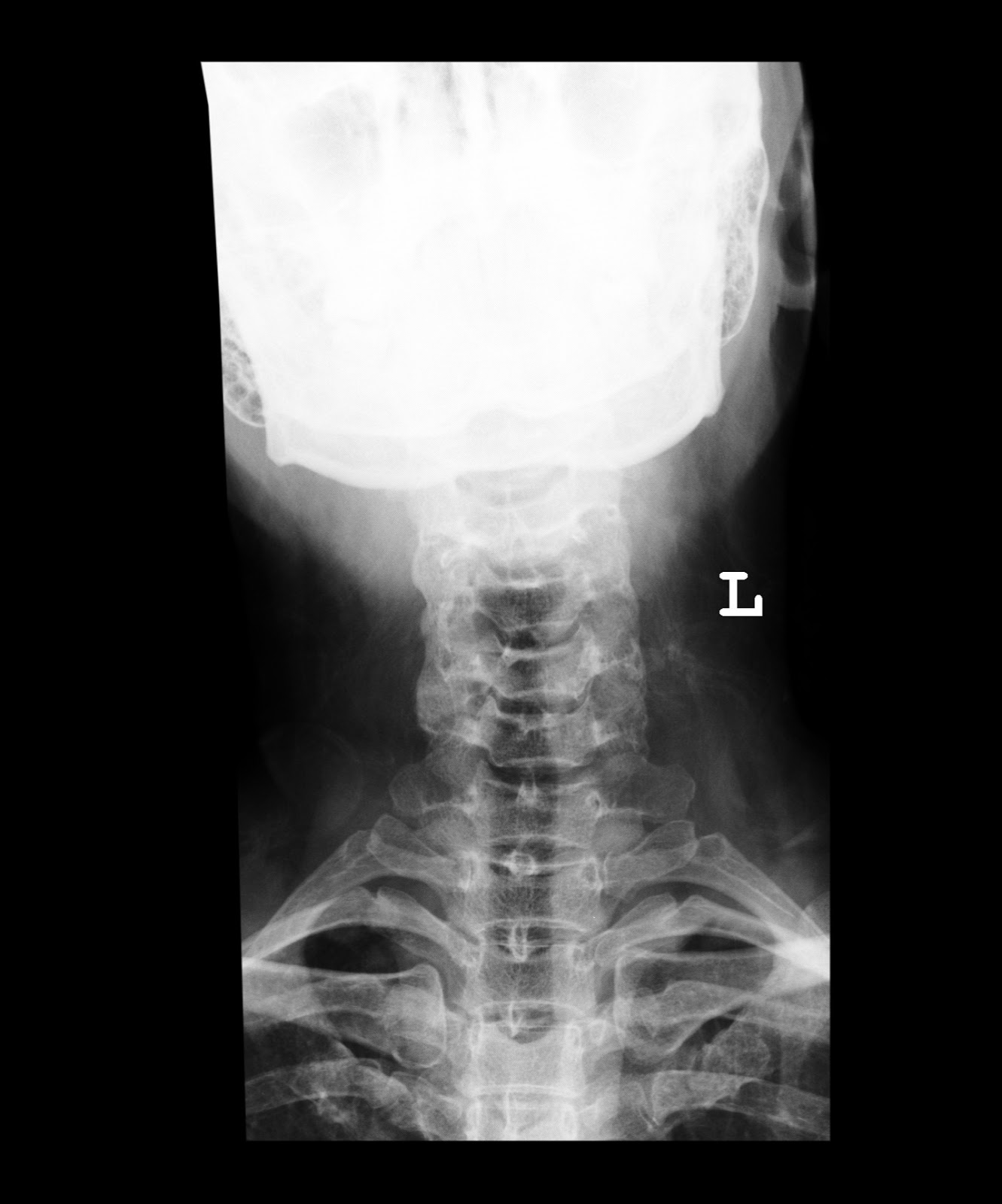
Radiographs (X-rays or conventional radiography) may be the first imaging tests a doctor performs when they suspect spondylitis. Radiographic axSpA - also called ankylosing spondylitis - refers to spondylitis that has progressed and caused visible bone changes on X-rays. Nonradiographic axial spondylitis refers to an early stage of the disease before bone changes can be seen by X-ray. The various types of spondylitis fall into two categories or disease stages: radiographic (X-rays) or nonradiographic. These tests can also be used to track the progression of the disease and monitor how effectively a current treatment is working. Following are some of the imaging tests used to confirm a diagnosis of spondylitis. 
0 Comments
Leave a Reply. |
Details
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
